
Type 1 diabetes (T1D) occurs when the body’s immune system attacks the insulin-producing beta cells in the pancreas. But this doesn’t happen overnight—instead, it’s a gradual process of beta cell loss over time.
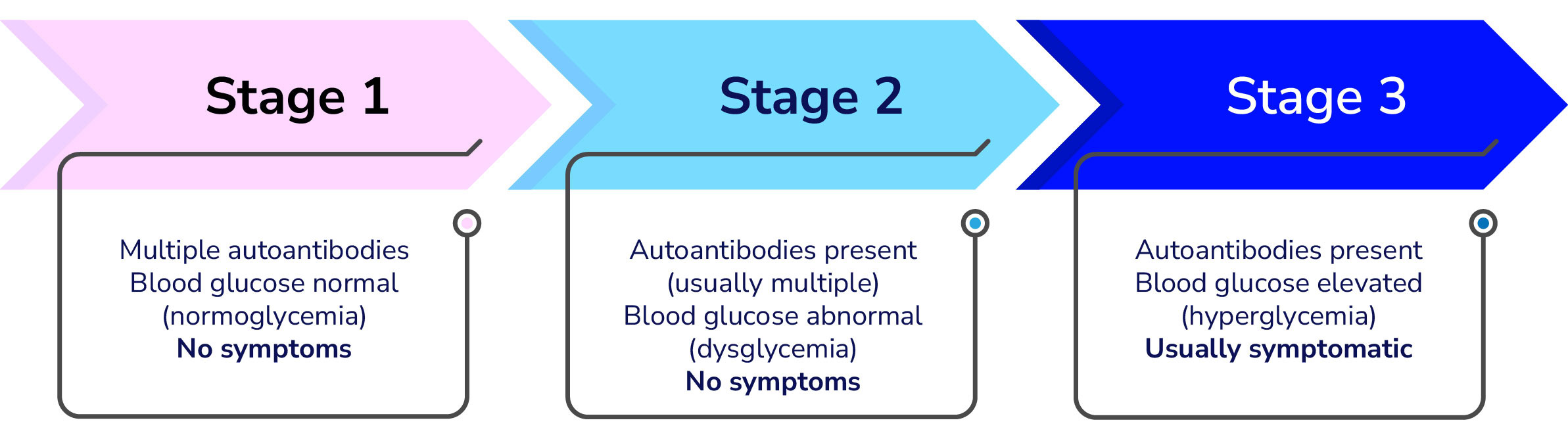
As the immune system attacks and destroys more beta cells, insulin production decreases, leading to abnormal blood-sugar levels. Eventually, enough beta cells are destroyed, and insulin production drops so low, that symptoms start to appear. Most people are diagnosed when these symptoms occur.
Insulin is an essential hormone that helps the body use the nutrients in our food as energy. Depending on how many beta cells are left in your body when your T1D is diagnosed, you may experience the honeymoon phase—which means you have a small number of beta cells that are still working and producing insulin.
Think of these remaining beta cells as a moderating force, helping you smooth out the peaks and valleys of managing T1D. That means you will likely need less insulin and may have an easier time reaching blood glucose targets.
Are some people more likely to experience the honeymoon phase?
The honeymoon phase is more common in (but not exclusive to) people who do not have diabetic ketoacidosis (DKA) at diagnosis, people with lower HbA1c levels at diagnosis, and children who are at least 5 years old.
How long does the honeymoon phase last?
The honeymoon phase is different for everyone! But it is always temporary. Generally, it lasts several months, but can be up to 1 to 2 years.
Is it possible to extend the honeymoon phase?
Currently, there are no FDA-approved therapies to extend the honeymoon phase. In the past decade, Breakthrough T1D has invested more than $273 million in research on disease-modifying therapies—which have the potential to slow, halt, prevent, or even reverse T1D onset—and several are in human clinical trials.
That includes baricitinib, a JAK inhibitor that interferes with signaling pathways critical to both immune cells and beta cells. In October 2025, Eli Lilly announced it was launching a new phase 3 clinical trial of baricitinib to examine whether the drug can preserve beta cell function in people with newly diagnosed T1D, which could potentially extend the honeymoon phase. Breakthrough T1D funded an earlier clinical trial investigating this therapy that helped make this next step possible.
What happens next?
Unfortunately, the honeymoon phase does not last forever. Even though this is a gradual process, eventually your immune system will destroy most or all of the beta cells in your pancreas. That means your daily insulin needs will gradually increase, and you may have more trouble managing your blood glucose levels.
It’s important to stay in contact with your T1D care team—they can help you make adjustments so you can reach your T1D management goals!